Findings: Recognizing Acute Right Heart Strain with POCUS: The D-Sign in Pulmonary Embolism
March 6, 2026 //
Tatiana Havryliuk, MD
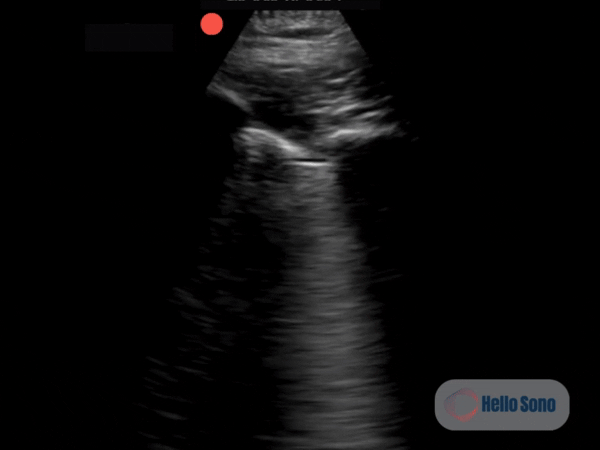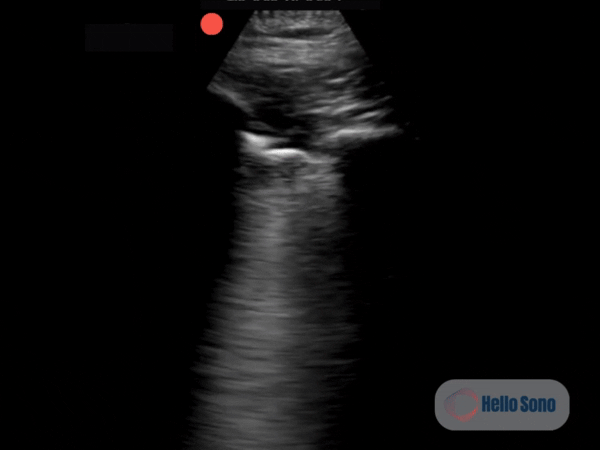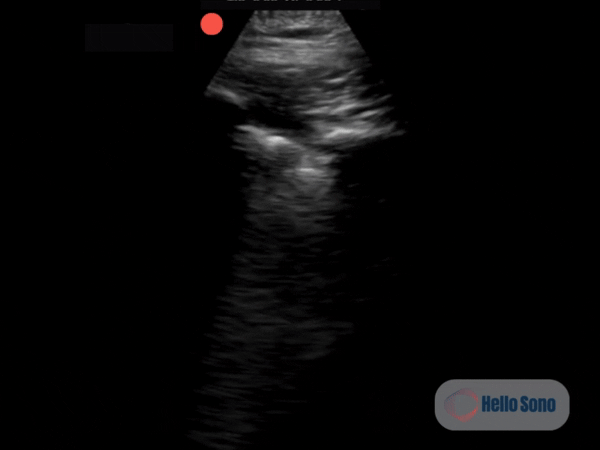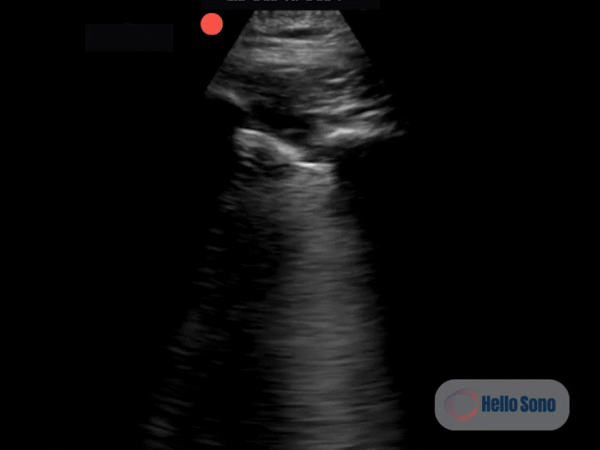
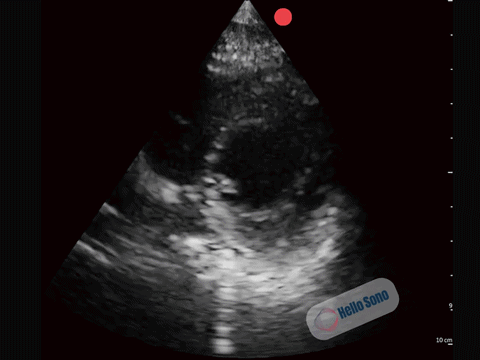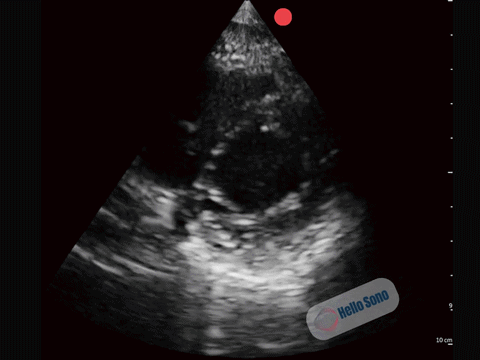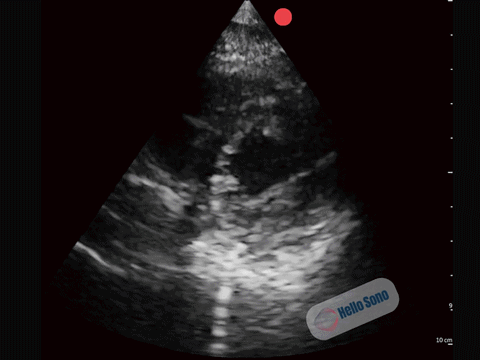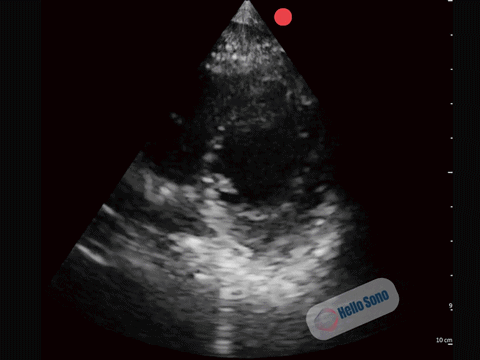
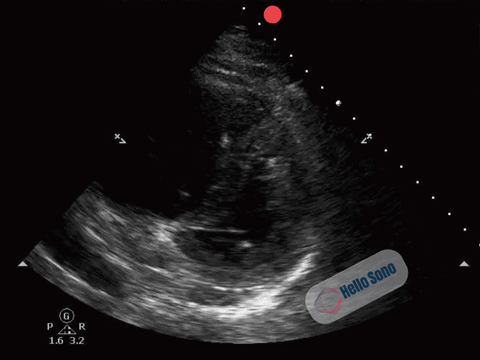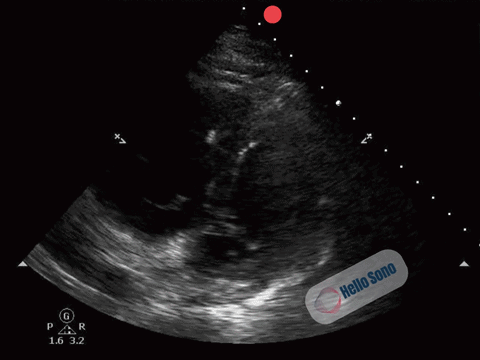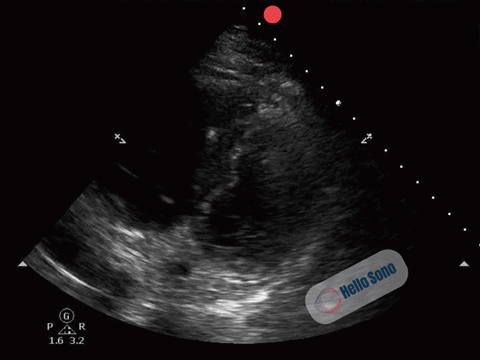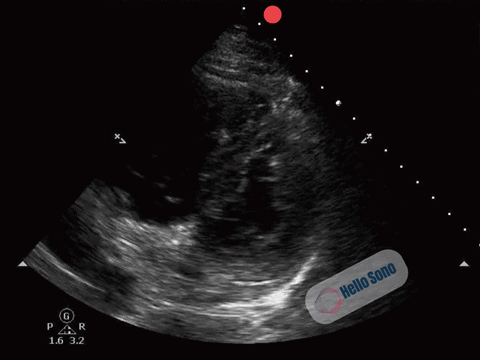 Clip 1. Parasternal short-axis view demonstrating right ventricular enlargement (right side of the screen) and septal flattening, resulting in a D-shaped left ventricle consistent with right ventricular pressure overload.
Clip 1. Parasternal short-axis view demonstrating right ventricular enlargement (right side of the screen) and septal flattening, resulting in a D-shaped left ventricle consistent with right ventricular pressure overload.POCUS Findings
The PSSA view demonstrates a flattened interventricular septum, creating a D-shaped left ventricle instead of the normal circular contour.
In addition, the right ventricle (RV) appears enlarged relative to the left ventricle on this view. The RV cavity occupies a larger proportion of the image than expected.
The combination of RV enlargement and septal flattening reflects acute right ventricular pressure overload.
In the appropriate clinical context, these findings are highly concerning for acute PE.
What a Normal POCUS Should Show
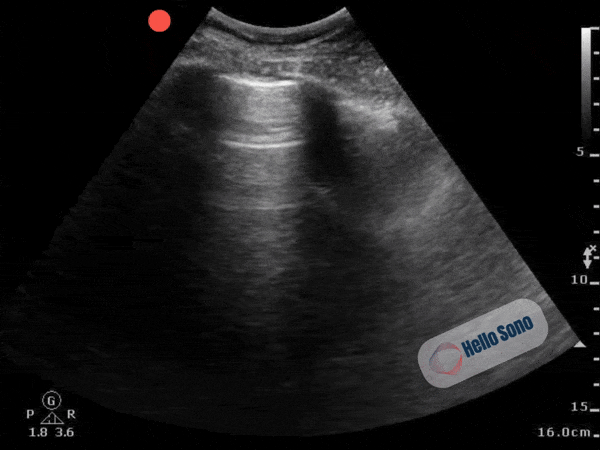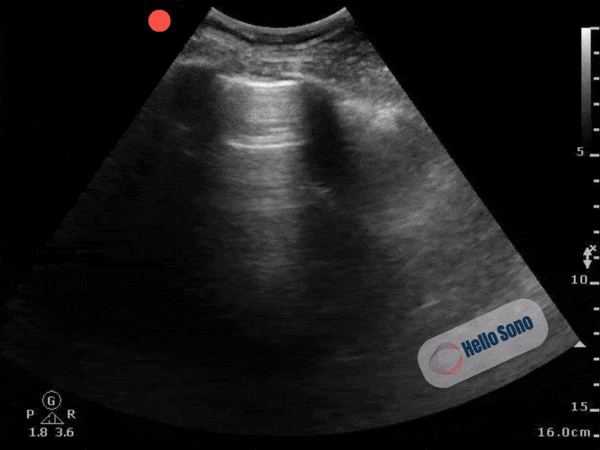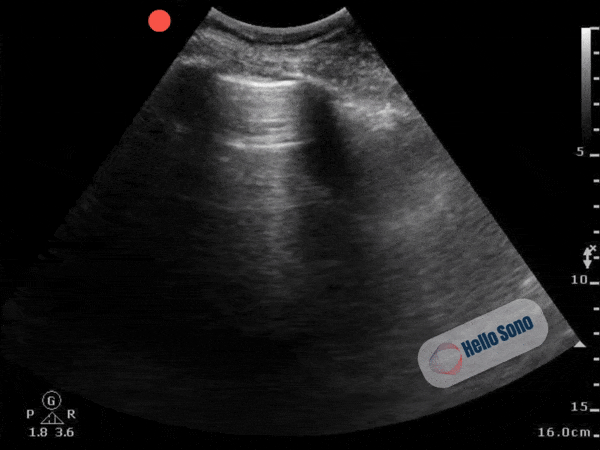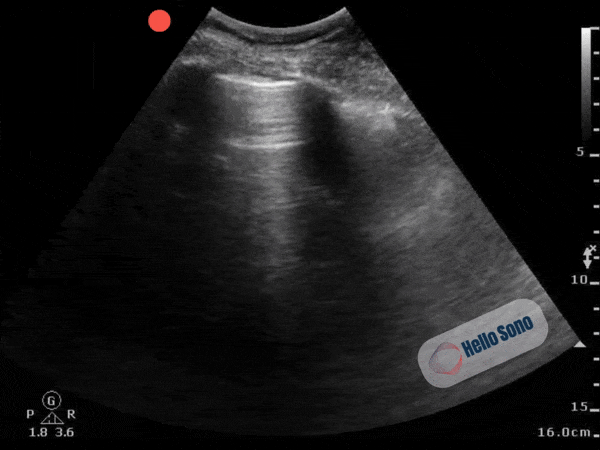
 Clip 2. Normal parasternal short-axis view at the level of the papillary muscles.
Clip 2. Normal parasternal short-axis view at the level of the papillary muscles.In a normal PSSA view:
- The left ventricle appears circular
- The interventricular septum maintains its natural curvature
- The right ventricle is clearly smaller than the left ventricle
The left ventricle should resemble a symmetric donut. When it takes on a D-shape, right-sided pressures are elevated.
Clinical Reasoning
Acute pulmonary embolism causes obstruction of pulmonary arterial flow, leading to a sudden increase in RV afterload. The thin-walled RV is not designed to tolerate this abrupt pressure rise, resulting in dilation and septal shift.
The D-sign is not diagnostic of PE in isolation. It indicates RV pressure overload. Clinical context determines the likelihood of PE.
In this patient with acute dyspnea, pleuritic chest pain, tachycardia, and OCP use, the finding significantly increases suspicion.
Here are other findings on cardiac POCUS that may be present in patients with an acute PE with RV dysfunction:
- McConnell's sign: Akinesia of RV mid-free wall with hypercontractility of the apex (distinctive for massive PE)
- Reduced TAPSE (tricuspid annular plane systolic excursion): <16-20 mm
- 60/60 sign: RV outflow tract acceleration time <60 ms with pulmonary arterial systolic pressure <60 mm Hg
- Visible RV or pulmonary artery thrombus (rare but diagnostic)
Evidence & Clinical Use of Cardiac POCUS in Pulmonary Embolism
Diagnosis:
Focused cardiac ultrasound is not sensitive enough to rule out PE in stable patients. However, the presence of RV strain increases specificity, particularly in moderate to large PE.
The American College of Physicians guidelines note that POCUS (lung, heart, IVC, and deep veins) added to standard diagnostic pathways correctly identified 89-100% of patients with PE and 95-100% without PE in patients with acute dyspnea.
In our patient, identification of a proximal DVT in the presence of RV strain would make PE highly likely, even before CT confirmation.
Risk Stratification:
Cardiac POCUS is central to risk stratification once PE is diagnosed, particularly for distinguishing intermediate-risk from low-risk PE in hemodynamically stable patients. Detection of RV dysfunction defines intermediate-risk PE and identifies patients at increased risk of hypotension, cardiogenic shock, and death.
Management:
In addition, there is consensus across professional societies to initiate empiric therapeutic anticoagulation while awaiting confirmatory testing in patients with intermediate or high pretest probability of PE, provided bleeding risk is low. Preemptive anticoagulation in intermediate and high probability patients has been shown to have a mortality benefit when diagnostic delay exceeds 2.3 hours for intermediate probability and 0.3 hours for high probability patients.
Case Resolution
The patient was treated with enoxaparin while awaiting confirmation of her diagnosis, given a high pretest probability for PE. CT pulmonary angiography confirmed bilateral pulmonary emboli with a large clot burden and RV enlargement.
She was diagnosed with intermediate-risk (“submassive”) PE and admitted to the telemetry floor for close monitoring for the next 48 hours.
Early bedside recognition of right heart strain expedited definitive imaging and appropriate inpatient management.
Impact of POCUS
In this case, a brief, structured ultrasound assessment:
- Excluded pneumothorax as a cause of pleuritic chest pain
- Identified RV strain
- Supported urgent imaging and initiation of anticoagulation
- Facilitated early admission and monitoring
By accelerating diagnosis and therapy, POCUS likely reduced the risk of clinical decline and potential ICU-level care.
Conclusion
In patients with acute dyspnea and pleuritic chest pain, time-sensitive decisions must often be made before definitive imaging is available. In this case, lung ultrasound ruled out pneumothorax, and cardiac POCUS revealed right ventricular strain on the parasternal short-axis view, substantially increasing the likelihood of pulmonary embolism.
By identifying right heart strain early, the clinician was able to initiate anticoagulation, expedite confirmatory imaging, and ensure appropriate monitoring. This case illustrates how cardiac POCUS in pulmonary embolism can sharpen clinical reasoning, strengthen risk stratification, and influence management in real time.
For practices considering implementing or expanding POCUS programs, tools such as POCUS ROI Calculators and a POCUS Billing Readiness Checklist can help estimate financial impact and ensure appropriate workflow and documentation processes are in place.
References
- Piazza G. Advanced Management of Intermediate- and High-Risk Pulmonary Embolism: JACC Focus Seminar. J Am Coll Cardiol. 2020;76(18):2117-2127. doi:10.1016/j.jacc.2020.05.028
- Poor H, Serrao G, Grapsa J, et al. High-Risk Pulmonary Embolism During Labor: JACC Patient Care Pathways. J Am Coll Cardiol. 2023;81(3):283-291. doi:10.1016/j.jacc.2022.10.004
- Falster C, Hellfritzsch M, Gaist TA, et al. Comparison of international guideline recommendations for the diagnosis of pulmonary embolism. Lancet Haematol. 2023;10(11):e922-e935. doi:10.1016/S2352-3026(23)00181-3
- Qaseem A, Etxeandia-Ikobaltzeta I, Mustafa RA, et al. Appropriate Use of Point-of-Care Ultrasonography in Patients With Acute Dyspnea in Emergency Department or Inpatient Settings: A Clinical Guideline From the American College of Physicians. Ann Intern Med. 2021;174(7):985-993. doi:10.7326/M20-7844
- Giri J, Sista AK, Weinberg I, et al. Interventional Therapies for Acute Pulmonary Embolism: Current Status and Principles for the Development of Novel Evidence: A Scientific Statement From the American Heart Association. Circulation. 2019;140(20):e774-e801. doi:10.1161/CIR.0000000000000707
- Blondon M, Righini M, Aujesky D, Le Gal G, Perrier A. Usefulness of preemptive anticoagulation in patients with suspected pulmonary embolism: a decision analysis. Chest. 2012;142(3):697-703. doi:10.1378/chest.11-2694
About the Author
Dr. Havryliuk is an emergency physician with over 15 years of clinical point-of-care ultrasound (POCUS) experience, a past Emergency Ultrasound Director at Brooklyn Hospital in NY, and the founder of Hello Sono. She is on a mission to empower clinicians with POCUS to take better and more efficient care of their patients by addressing two key barriers, lack of competency and infrastructure.
Learn more at www.hellosono.com
LinkedIn: https://www.linkedin.com/in/tatiana-havryliuk-md/
Email: [email protected]
*POCUS images and graphics provided courtesy of Hello Sono.